Digital Smile Design: The Future of Aesthetic Dentistry
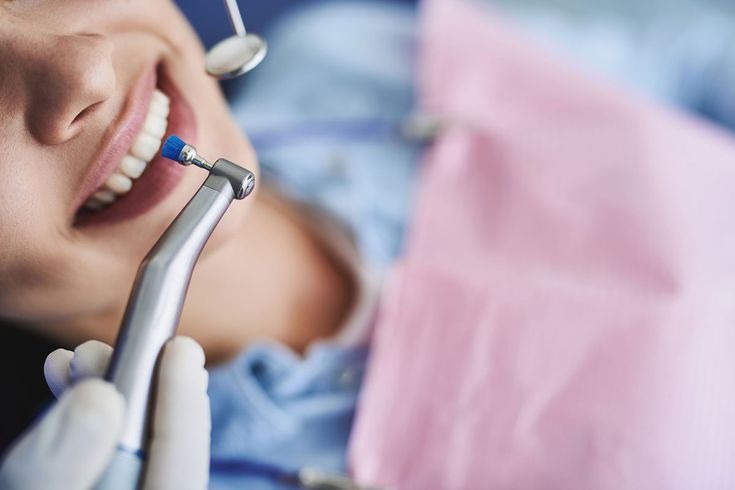
Digitalization has now assumed an important aspect not only in engineering but also in the dental field. Digital Smile Design (DSD) is a modern versatile innovative dental treatment planning tool invented by the Brazilian dentist Christian Coachman in 2007 that permits the professional in digitally design the smile of the patient from a series of pre- and post-DSD photographs.
DSD software also allows the clinician to educate the patients regarding the improvements that can be done and also helps in collecting the patient’s own preferences and requirements, thereby making the patient feel like he is a part of the decision-making process rather than just being on the receiving end. DSD was described by its developers Christian Coachman and Marcelo Calamita as an innovative multipurpose analytical software that is capable of diagnosis, performing meticulous analysis of the patient’s facial and dental traits that may have eluded conventional photography and the human eye.
Aesthetic dentistry has become one of the most sought-after disciplines in dentistry which focuses on the smile and pleasing appearance. Modern dentistry is not limited to just the repair of individual teeth. There has been an increase in the incidence of patients who give aesthetic outcomes the main priority with the restoration of the tooth structure.
An aesthetic makeover or smile design involves creating a smile where the stomatognathic structures function without hindrance to each other, a perfectly functioning orofacial structure compliments each other. Designing an aesthetic smile is very essential in formulating an aesthetic makeover.
PRINCIPLES OF SMILE DESIGNING
Designing a perfect smile using the software requires a thorough knowledge about the muscles and dimensions of the display zone along with their aesthetic proportions. Since not all individuals are alike, each person should evaluate and study with accurate detail in order to come up with their perfect smile. All these elements are connected with each other. Any change will definitely affect the other element.
Although a software algorithm is used in predicting a perfect smile, clinical smile designing requires a multidisciplinary intervention that includes branches of dentistry such as orthodontics, orthognathic surgery, periodontal therapy, and plastic surgery.
EVOLUTION OF SMILE DESIGN
Before the invention of photoshop and advanced photo tracers, perfect smile lines were drawn by hand and then printed over the photos of the patient and would often be discussed with patients for their input. This process has now been largely replaced by smile automation software, referred to as Digital Smile Design (DSD) software, all of which with the click of a button tells us the modifications needed to be executed in order to get a perfect smile. Some of the key milestones in the evolution of smile design include:
Generation 1. Manual hand drawings using pencil markers were made over the patient’s full profile photographs. The drawback of this method was that if taken with a study model, the correlation between the patient’s full profile photo and study model was very poor.
Generation 2. With the creation of Microsoft Office, drawings were often done digitally and then correlated with the model. This helped in tracing minor modifications that needed to be done. Diagrams were often 99% accurate.
Generation 3. The next generation enabled the two-dimensional (2D) drawings to be linked with physical analog models which permitted a wax-up of the final smile.
Generation 4. The 2D drawings were written up into an algorithm that was then processed digitally and this step enabled the technique of facial 3D analysis, also determining the facial components and aesthetic parameters.
Generation 5. Innovation of intraoral camera which allowed us to scan and take digital impressions which were more accurate than impressions taken with any other conventional method.
Generation 6. Introduction of 4D where digital sensors placed on the patient’s jaw captures the smile motion and movement inside the 3D environment using the MODJAW software and designing the smile with CAD/CAM technology. This technology reduces the need for changes, including reduced tooth preparation and other issues by testing the design with the real movement of the jaw.
REQUIREMENTS OF DIGITAL SMILE DESIGN
Some of the software that can be used for digital smile design include Photoshop (Adobe), Microsoft PowerPoint (Microsoft Office, Microsoft), Smile Designer Pro (SDP) (Tasty Tech Ltd), Aesthetic Digital Smile Design (ADSD – Dr. Valerio Bini), DSD App by Coachman (DSDApp LLC), Keynote (iWork, Apple, Cupertino, California, USA), NemoDSD (3D) and Exocad DentalCAD, a digital SLR camera.
A digital impression of both the jaws is taken with a digital intraoral scanner. The impressions are then uploaded to the CAD/CAM processing machine where they are 3D-printed.High-resolution full profile photographs representing the facial profile and frontal views of the patient are essential and videos that record the dynamic changes of the teeth, gingiva, lips, and facial muscles brought about by smiling and talking are essential as this documentation forms the blueprint on which smile design is executed. Three basic photographic views are fundamental in smile design, they include
- Full facial view with a natural smile.
- Resting face.
- A view representing the maxillary and mandibular arch not in occlusion.
A magnification of a 1:1 view picture of the central incisor with a black background provides in-depth detail for the lab technician to work on. The videographic demonstration containing documentation is imported into the slide presentation. The facial and dental components of the smile and their points previously discussed above influence the majority of smile design. Commercially available DSD software include; CEREC Smile Design (SIRONA), Digital Smile System (DSS), Smile Design Pro (TASTY TECH), G Design (HACK DENTAL), Romexis Smile Design (PLANMECA), and Smile Composer (3 SHAPE).
DSD WORKFLOW
The DSD workflow begins with digital scanning of the patient’s dentition using an intraoral scanner, which is then imported to the respective DSD software. Using the various different shapes and forms available in the digital repository, we can overlap the teeth for a given aesthetic procedure. The DSD workflow then proceeds as follows:
- After uploading the facial photographs, two baselines are drawn on the centre of the slide so that it forms a + sign, in a way that it appears to be placed between the upper and lower anterior with the teeth apart. Horizontal reference lines are achieved through the interpupillary line creating a digital facebow.
- Soft tissue features (gingiva, lips, facial lines) and their association with other components are evaluated by grouping and transferring them to the facial photograph.
- A template tooth that is set to be standard and exact in dimensions is placed over the original photograph so that axial inclinations, proportion in relation to adjacent teeth, and soft tissue silhouette are established. The retracted view is engaged in order to evaluate whether the intraoral photograph is concurrent with facial baseline data, where three lines are drawn:
Line 1: Intercanine width measured from the tip.
Line 2: The middle third of the central incisor to the occlusal edge of the adjacent central incisor.
Line 3: From the philtrum of the upper lip to the interdental papilla and the incisal embrasure.
- Rectangular crop mode is then chosen and placed over the region of both central incisors to measure the width/length proportion of the central incisors.
- Using editing tools, the template tooth can be placed over the photographed tooth, and pasted and morphed according to the best esthetic outcome. The patient’s preferences and inputs can also be gathered and included during this step.
- A digital ruler available in the software can be used to calibrate the real-time dimensions of the tooth by recording the measurement on the 3D model and then incorporating it into the software. Gingival contour and the proportion to attached gingiva width and incisal edges can also be calibrated.
- Transferring the + sign to the cast: The measurement of baseline point till the free gingival margin is recorded and then transferred to the 3D cast with the aid of a calliper. Horizontal lines above the teeth which predict the gingival margin are marked on the cast using a pencil mark. The vertical lines are then marked using the interval between the incisal embrasures along with the facial component, which is then marked in the 3D model.
- Wax up of the procedure to be performed for establishing a smile and then carried out on the cast and evaluated using DSD, after which it is tried on the patient.
- Once the approval of the wax-up has been sought, minor corrections, if deemed necessary, are performed.
- Minimal intervention should be prioritized such as minimal reduction of tooth surfaces, and giving proper clearance for crowns, if required. Attention to detail in each step in DSD usually results in an outcome that goes beyond the patient’s expectations.
ADVANTAGES OF DSD
DSD enables the patient to actively participate in their treatment plan, resulting in much higher compliance and better motivation, as the results are evident from the 3D previsualization and simulation. The changes can be customized according to their desires. Digital scanning allows the clinician to detect any insidious disease due to the relatively high shades of gray (256 pixels) compared to a conventional radiograph (16–25 pixels).
CONCLUSION
The DSD is an innovative tool that helps the clinician to create aesthetically pleasing smiles. Previsualization drastically increases the patient’s acceptance rate. The technology also makes the patient a part of the decision-making process by including their preferences. Although caution should be exercised that ideal case selection is always necessary in order to have a successful outcome. Patients should be enlightened about the potential ups and downs that they might face if the results are not up to their expectations.
Diabetes
People with diabetes are more likely to have periodontal disease than people without diabetes, probably because people with diabetes are more susceptible to contracting infections. In fact, periodontal disease is often considered a complication of diabetes. Those who don’t have their diabetes under control are especially at risk. Research has suggested that the relationship between diabetes and periodontal disease goes both ways: periodontal disease may also make it more difficult for people who have diabetes to control their blood sugar, increasing the risk for diabetic complications.
Heart Disease
Several studies have shown that periodontal disease may increase the risk of heart disease. Scientists believe that inflammation caused by periodontal disease may be responsible for the association. Periodontal disease can also exacerbate existing heart conditions. Patients at risk for infective endocarditis may require antibiotics prior to dental procedures. Your periodontist and cardiologist will be able to determine if your heart condition requires use of antibiotics prior to dental procedures.
Respiratory Disease
Research has found that bacteria associated with periodontal disease can be aspirated into the lungs and contribute to respiratory diseases such as pneumonia.
Cancer
Researchers found that men with gum disease were 49% more likely to develop kidney cancer, 54% more likely to develop pancreatic cancer, and 30% more likely to develop blood cancers.
Alzheimer’s Disease
Studies have shown a connection between bacteria associated with periodontal disease and the progression of Alzheimer’s disease. Gum disease bacteria may be able to travel to the brain and contribute to the development of Alzheimer’s disease.

